Dream Team
THE COMBINATION OF EFFECT LIQUIDS AND MICRO-LAYERING ON HIGHLY AESTHETIC ZIRCONIA IS THE EFFECTIVE WAY TO ACHIEVE OUTSTANDING RESULTS
Case by Leonidas Dimitriou, MDT
As an addition to its well-aligned portfolio of multi-layered zirconia (KATANA™ Zirconia Multi-Layered series) and veneering porcelain for zirconia (CERABIEN™ ZR), Kuraray Noritake Dental Inc. has recently introduced a set of dyeing liquids. Esthetic Colorant for KATANA™ Zirconia is applied to the surface of the monolithic or anatomically reduced zirconia restoration prior to the final sintering procedure. In this way, it is possible to imitate typical internal colour effects of natural teeth quite easily. Depending on the desired outcome, users may add just a final layer of glaze, liquid ceramics or stains and porcelains to their zirconia restorations treated with Esthetic Colorant. The following two case examples are used to demonstrate two different procedures involving the use of the effect liquids.
CASE EXAMPLE 1
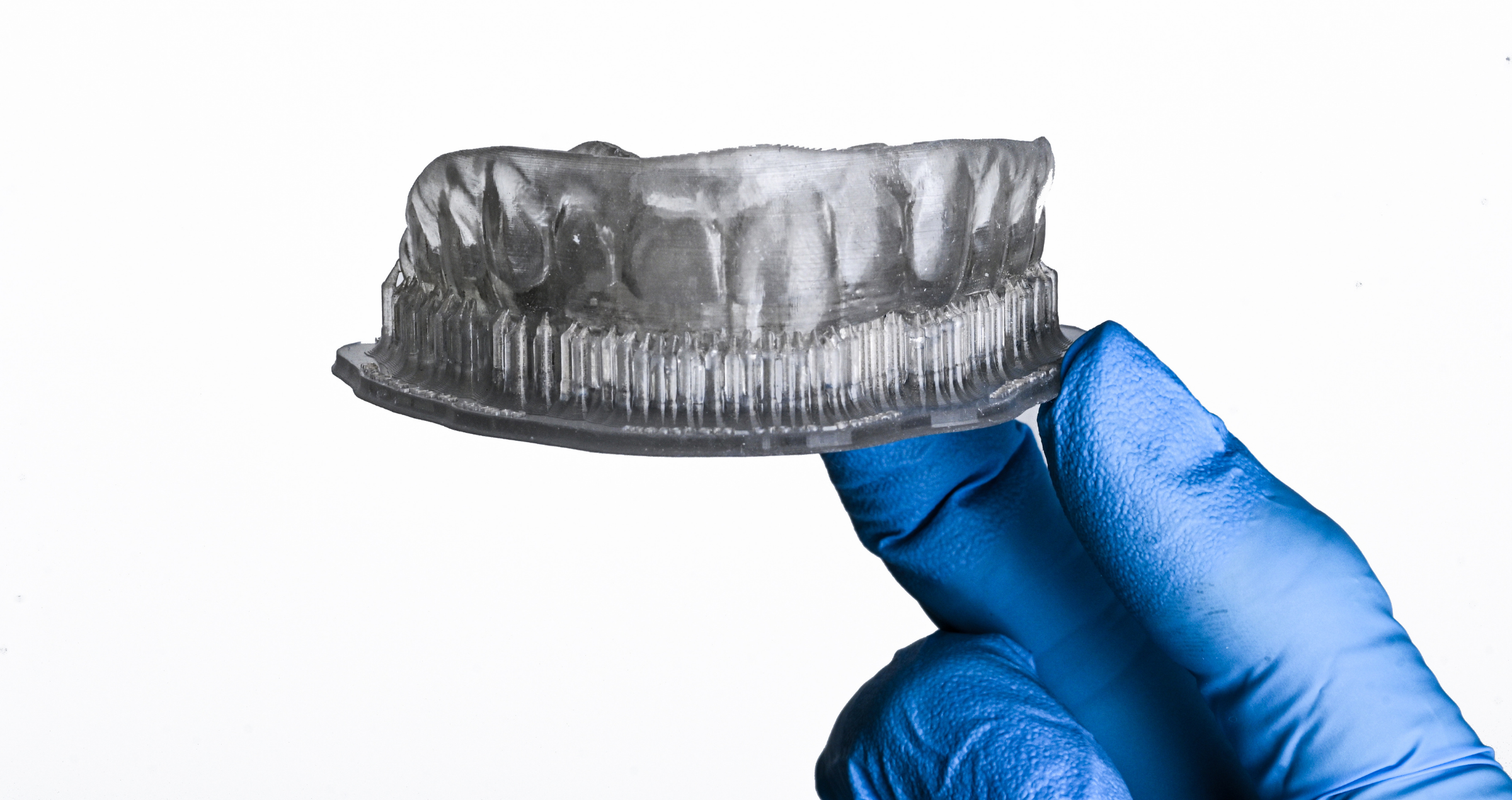
In the first case, we produced three two-unit splinted crown restorations for six maxillary anterior teeth. The zirconia crowns (made of KATANA™ Zirconia YML) were anatomically reduced and individualized with Esthetic Colorant mainly in the incisal and cervical areas immediately after milling. For the application of the selected liquids, we used the Liquid Brush Pen specifically developed for Esthetic Colorant. The restorations were dried for half an hour, placed in the sintering furnace for sintering according to the recommended protocol for KATANA™ Zirconia and subsequently finished with CERABIEN™ ZR porcelains. Finally, CERABIEN™ ZR Paste Stain Glaze was applied for the final high-gloss finish.
Fig. 1. Pre-sintered anatomically reduced crowns after milling.
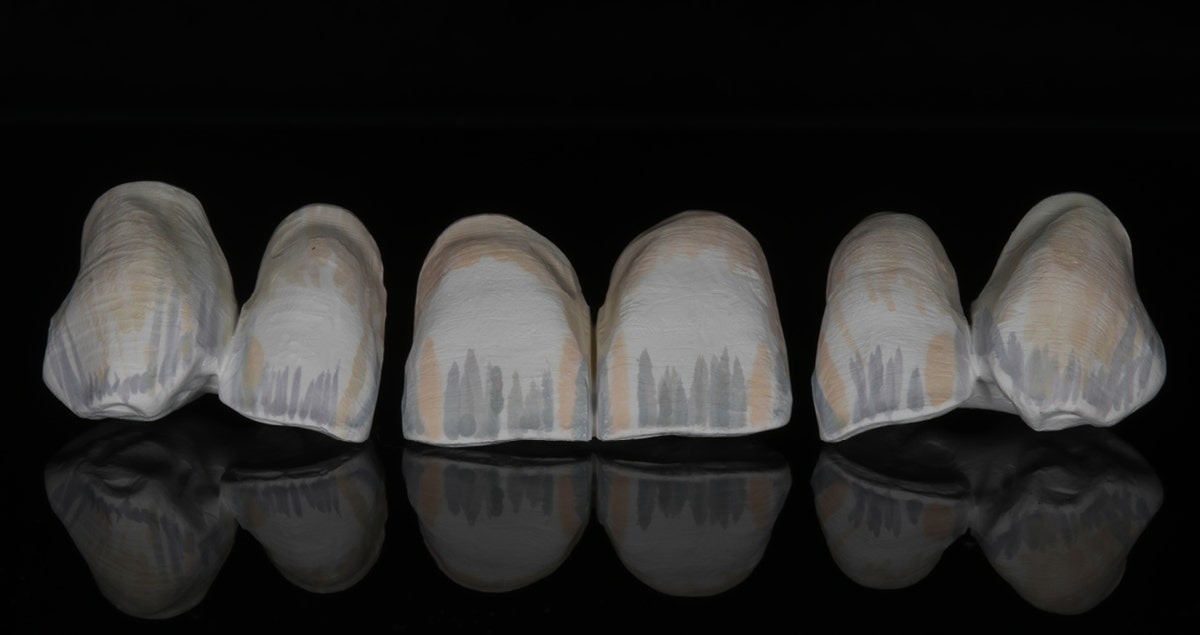
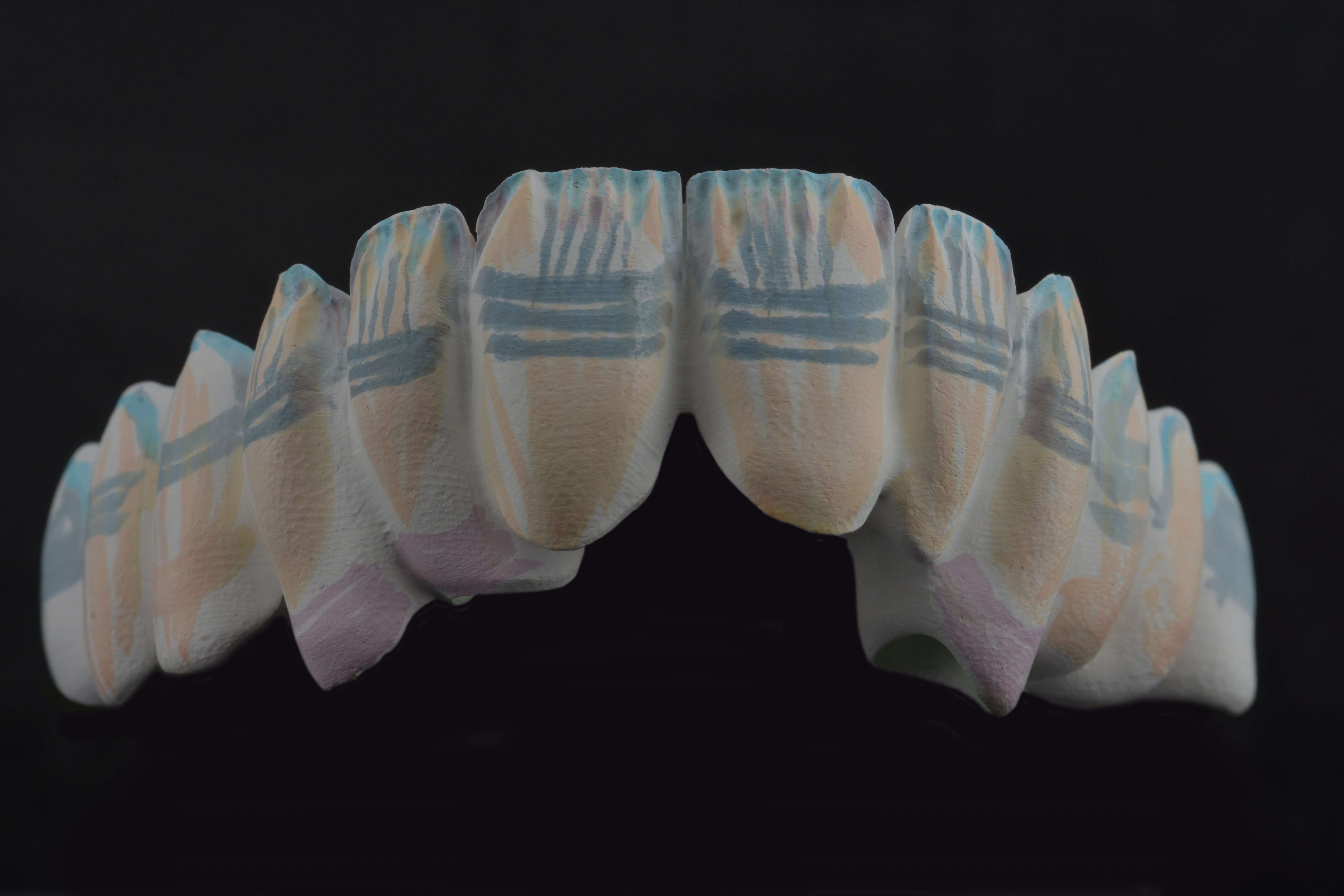
Fig. 2. Esthetic Colorant applied to the milled restorations.
Fig. 3. Appearance of the individualized restorations after the final sintering procedure.
Fig. 4. Restorations after porcelain layering.
FINAL SITUATION
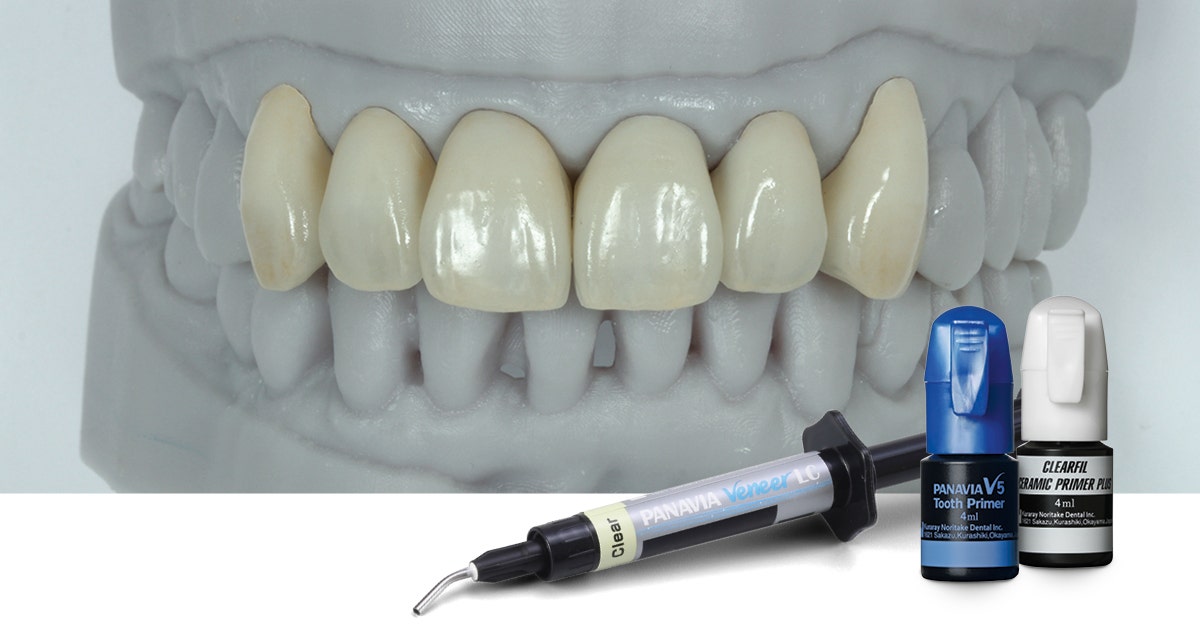
Fig. 5. Final restorations with a natural appearance. The effects created with Esthetic Colorant shine from deep within the restorations.
Fig. 6. Lateral view of the final restorations from the left.
Fig. 7. Lateral view of the final restorations from the right.
CASE EXAMPLE 2
In this second case, two three-unit restorations were produced using KATANA™ Zirconia YML in the colour A3. We designed and milled them in full contour, then reduced them with hand instruments by 0.2 mm and added some texture effects to the surface before applying Esthetic Colorant. In this case, we played with different shades of Esthetic Colorant. Even when applied on a minimally reduced or monolithic surface, the liquids are able to create a nice depth effect as they diffuse into the zirconia structure. The amount of liquid applied is easily controlled with the Liquid Brush Pen, so that the intensity of the colours is predictable. After sintering, we added some internal stains, CERABIEN™ ZR Luster Porcelain and a final layer of CERABIEN™ ZR FC Paste Stain Glaze to finish the restorations. The outcome speaks for itself.
Fig. 8. Milled monolithic restorations with a pronounced surface texture.
Fig. 9. Vestibular and palatal surfaces individualized with Esthetic Colorant to create and intensify some natural colour effects.
Fig. 10. Appearance of the restorations immediately after sintering.
Fig. 11. Restorations after internal staining.
Fig. 12. A layer of luster porcelain applied to the minimally reduced restorations.
FINAL SITUATION
Fig. 13. Final outcome after glazing.
Dentist:
LEONIDAS DIMITRIOU, MDT