Case by Dr. Ioannis Memis
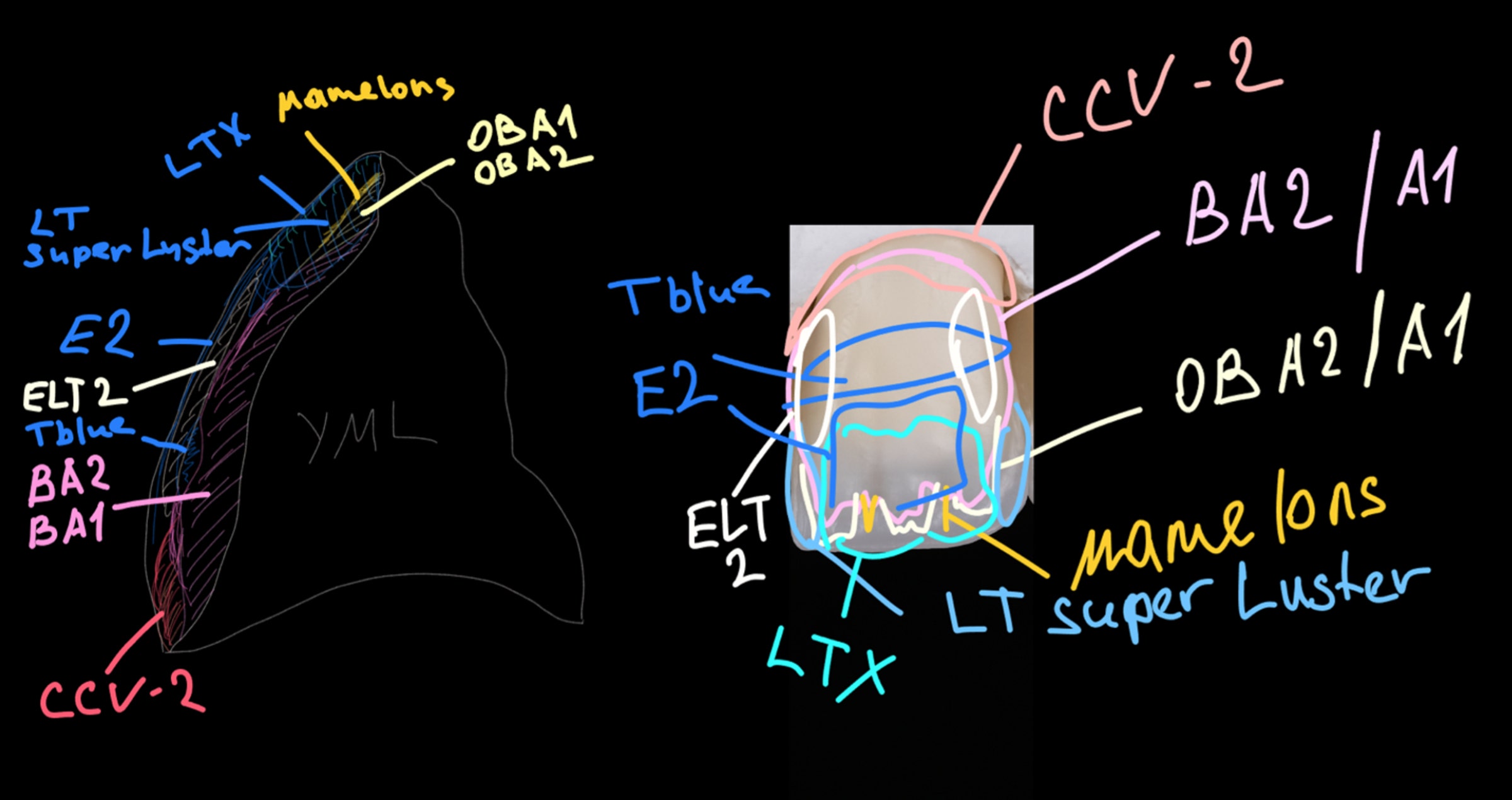
Single-shade or two-shade approach? Using modern resin composites, it is possible to treat virtually every patient in need of a direct restoration in an aesthetic way using one of those two techniques. If the defect is rather small, a single shade of composite restorative in a body opacity may be sufficient – especially when the tooth to be restored is in the posterior region. Larger defects and those located in the aesthetic zone may require a combination of two different shades – one as a dentin replacement and one as translucent as enamel – to closely imitate the optical characteristics of the natural tooth.
With CLEARFIL MAJESTY™ ES-2, Kuraray Noritake Dental Inc. offers a complete composite system designed to simplify procedures in bot, the single-shade and the two-shade approach. CLEARFIL MAJESTY™ ES-2 Classic is a typical composite for the single-shade technique consisting of 18 shades offered in a single universal opacity. Shade determination is brightness-based, meaning that the brightness is selected first and the hue and colour saturation in a second step (using the VITA Classical A1 – D4 shade guide). For those who want to skip shade determination completely, CLEARFIL MAJESTY™ ES-2 Universal has been introduced. It consists of only two shades for the anterior and one shade for the posterior region, selectable without using shade tabs. For the two-shade technique, CLEARFIL MAJESTY™ ES-2 Premium is the solution: It allows users to copy natural enamel and dentin layers with a total of seven enamel, seven dentin and four translucent shades. Its exceptional feature: pre-defined colour combinations with one Premium shade combination covering three VITA Classical shades. A natural blending into the environment is achieved with the Light Diffusion Technology in the formulation.
All three versions of CLEARFIL MAJESTY™ ES-2 are compatible with each other and offer the same favourable handling properties. The use of different techniques, shades and opacities is demonstrated using the following patient case.
YOUNG PATIENT WITH MULTIPLE CARIOUS LESIONS
A 24-year-old female patient was referred from undergraduate clinic of Operative Dentistry of the Aristotle’s University of Thessaloniki - School of Dentistry (Greece). Patient presented multiple interproximal carious lesions in need of restorative treatment. In the clinical and radiographic examination, the following defects were identified:
Quadrant 1 (maxillary right):
- Distal lesion on the lateral incisor (Class III)
- Mesial and distal lesions on the first premolar (Class II)
- Mesial and distal lesions on the second premolar (Class II)
- Mesial lesion on the first molar (Class II)
Quadrant 2 (maxillary left):
- Distal lesion on the lateral incisor (Class III)
- Mesial lesion on the first premolar (Class II)
- Mesial and distal lesions on the second premolar (both Class II)
- Mesial lesion on the first molar (Class II)
Quadrant 3 (mandibular left):
- Distal lesion on the first molar (Class II)
- Mesial lesion on the second molar (Class II)
In a stepwise procedure, the teeth were restored with CLEARFIL MAJESTY™ ES-2 either in a single-shade or in a two-shade approach depending on the size of the lesions.
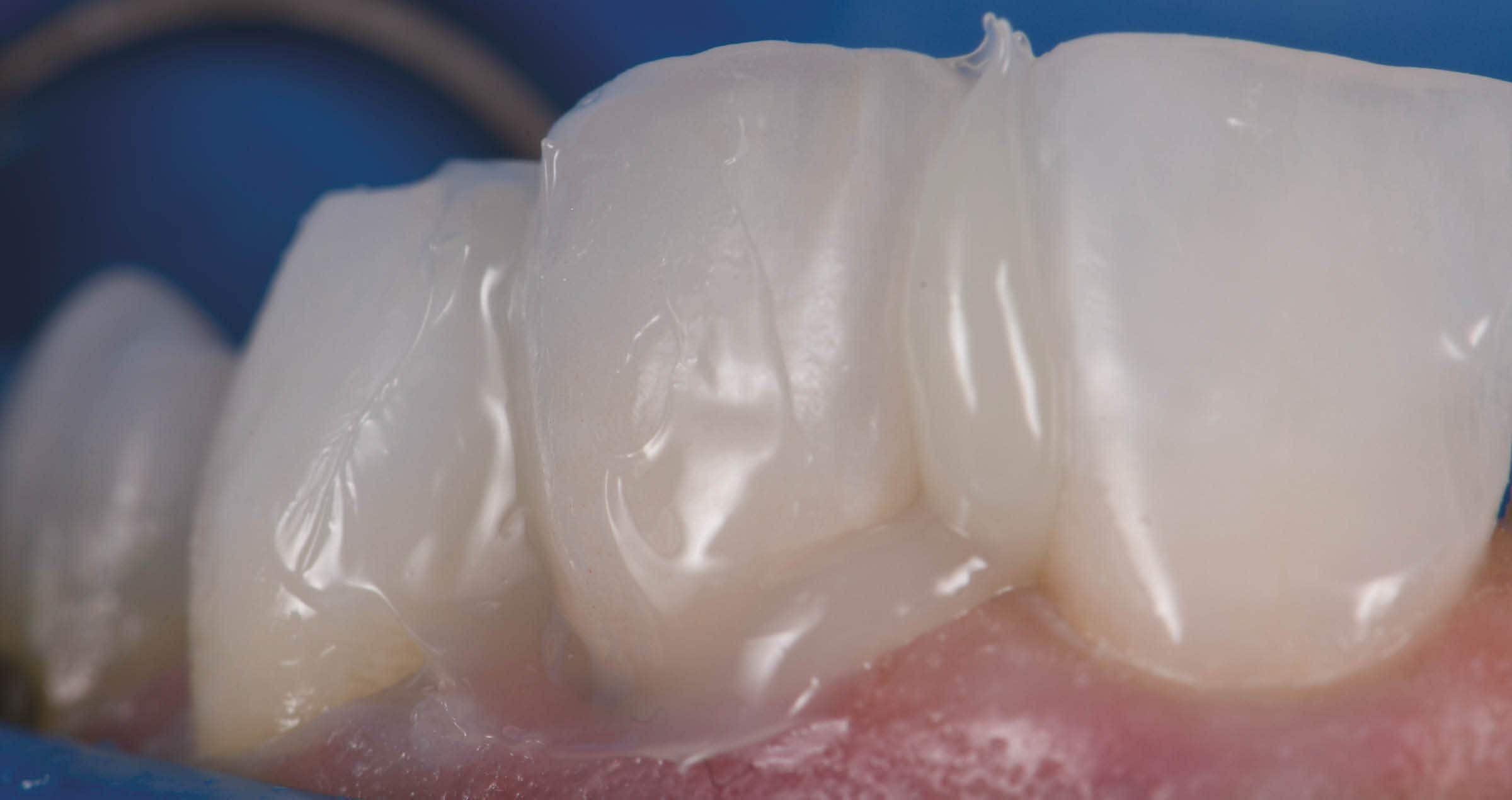
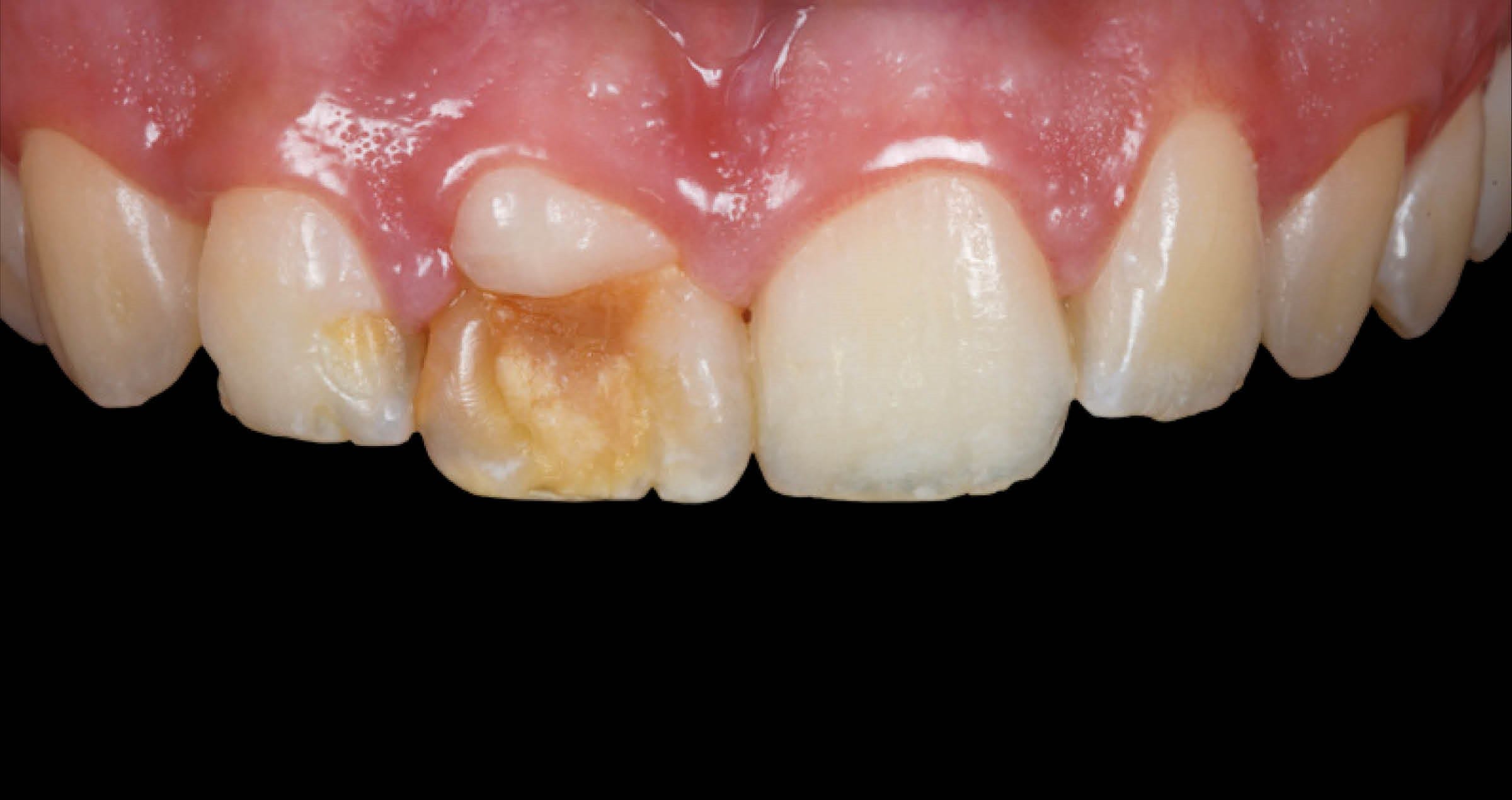
INITIAL SITUATION
Fig. 1. Initial situation: Frontal view.
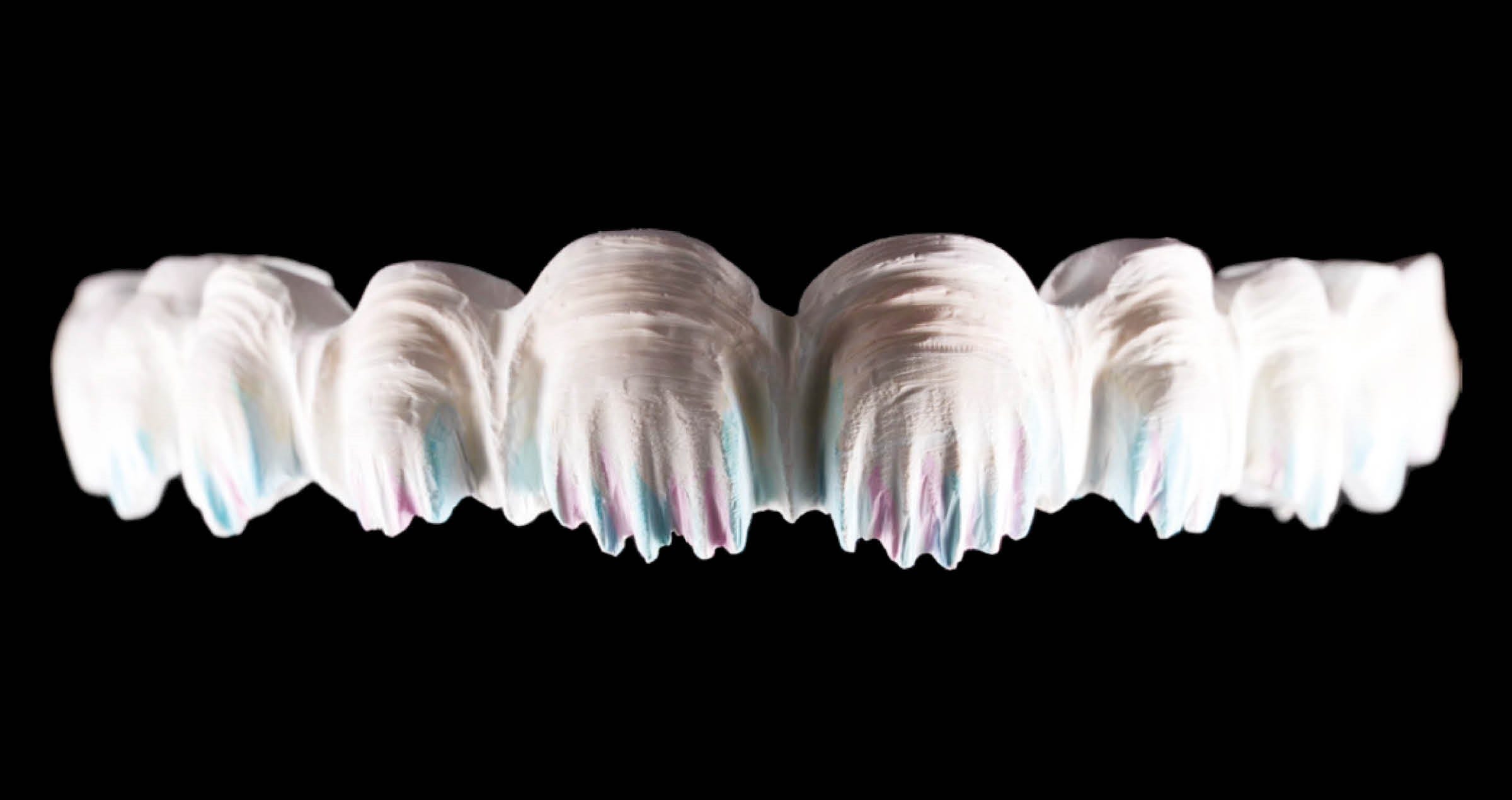
Fig. 2. Occlusal view of the maxilla.
Fig. 3. Occlusal view of the mandible.
RESTORING THE TEETH IN QUADRANT 1
The six carious lesions in this quadrant were restored in three steps. At first, the focus was on the first molar and second premolar. Opening the larger cavity mesially of the first molar provided access to the smaller lesion on the premolar’s distal surface. After caries excavation and cavity preparation, rubber dam was placed and fixed with a clamp on the second molar. The enamel in the cavities was treated with phosphoric acid etchant for 15 seconds before CLEARFIL™ Universal Bond Quick (Kuraray Noritake Dental Inc.) was applied according to the manufacturer’s instructions. For a morphologically correct designing of the proximal contact point and area, the use of a sectional matrix system with rings was utilized. Both cavities were restored with CLEARFIL MAJESTY™ ES-2 Premium in the shades A3D and A2E. Finishing and polishing of the occlusal surface accomplished with silicon cups and Twist Dia disks on a slow speed handpiece.
In the second step, the distal lesion on the first and mesial lesion on the second premolar were restored in an identical procedure with CLEARFIL MAJESTY™ ES-2 Premium in the shade A3D and CLEARFIL MAJESTY™ ES-2 Classic in the shade A3. A different approach was selected in step 3 for the lesions on the distal part of the lateral incisor and the mesial part of the first premolar. Due to the small size and the all-but-prominent position of the lesions, a single-shade technique using CLEARFIL MAJESTY™ ES-2 Classic in the shade A3 was selected. Between the lateral incisor and canine, a posterior sectional matrix was placed in an upright position and fixed with a wedge to support a proper restoration of the contact point, while both elements were used in the usual way between the canine and first premolar.
Fig. 4. Simultaneous restoration of the mesial lesion on the first molar and the distal lesion on the second premolar with CLEARFIL MAJESTY™ ES-2 Premium.
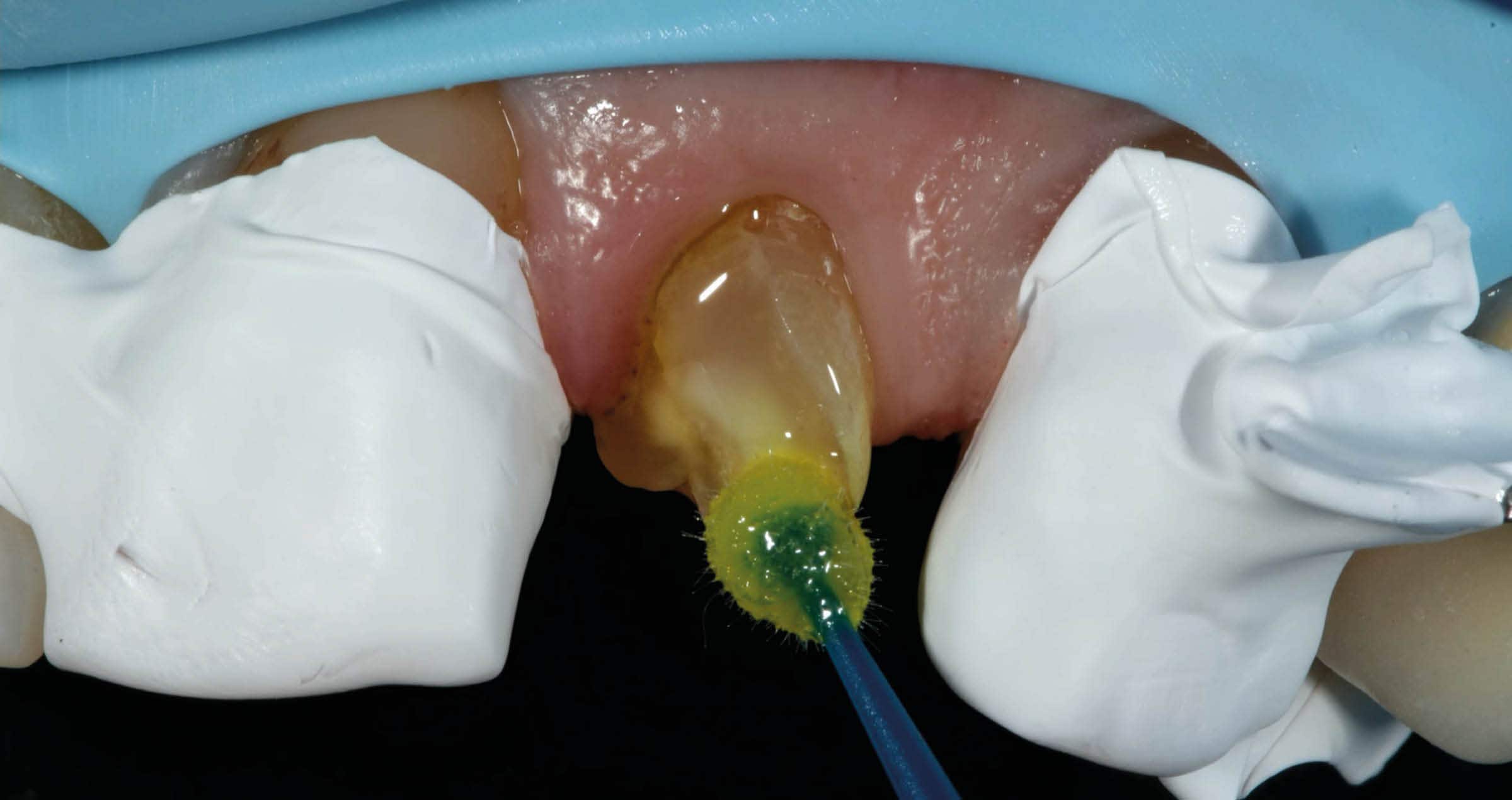
Fig. 5. Restoration of the distal lesion on the lateral incisor and the mesial lesion on the first premolar with CLEARFIL MAJESTY™ ES-2 Classic.
RESTORING THE TEETH IN QUADRANT 2
For the small disto-palatal lesion on the maxillary left lateral incisor, a single-shade technique with CLEARFIL MAJESTY™ ES-2 Classic in the shade A3 also produced aesthetic outcomes. The four lesions at the posterior region of the quadrant were restored in two steps – one for each pair of proximal lesions – with a combination of CLEARFIL MAJESTY™ ES-2 Premium in the shade A3D and CLEARFIL MAJESTY™ ES-2 Classic in the shade A1.
Fig. 6. A single-shade technique is sufficient to aesthetically restore this small lesion on the left lateral incisor.
Fig. 7. Simultaneous restoration of the mesial lesion on the second premolar and the distal lesion on the first premolar.
Fig. 8. Simultaneous restoration of the mesial lesion on the first molar and distal lesion on the second premolar.
RESTORING THE TEETH IN QUADRANT 3
In this quadrant, only a single pair of proximal lesions needed treatment. A simultaneous restoration procedure was selected once again due to the favourable space conditions. Although the size of the lesion was like those in the posterior region of the maxilla, a single-shade restoration was selected with the use of CLEARFIL MAJESTY™ ES-2 Classic (shade A3).
Fig. 9. Treatment of the lesions in quadrant 3.
CONCLUSION
In the present patient case, several different shades, opacities, and combinations of CLEARFIL MAJESTY™ ES-2 were utilized either in a single- or in a two-shade approach. All combinations and techniques produced good outcomes. As shown in Figure 4, the enamel opacity of CLEARFIL MAJESTY™ ES-2 Premium is visibly more translucent than the universal opacity of CLEARFIL MAJESTY™ ES-2 Classic. Experience shows that enamel shades translucency is highly valuable for aesthetic anterior restorations, while in posterior restorations, the universal shade approach is aesthetically adequate, particularly for medium-sized restorations, as shown in Figure 9. This is clearly an evidence of Light Diffusion Technology which is blending hue and colour saturation to the surrounding tooth structure.
Handling of all selected composite pastes is comfortable: non-sticky, adaptable to cavity walls and allowing precise occlusal sculpting. Polishing with Silicone Cups and TWIST DIA for Composite is easy, quick and leaves a natural gloss on the surface.Dentist:
DR. IOANNIS MEMIS
Postgraduate Student, Operative Dentistry Dept., School of Dentistry
Aristotle University of Thessaloniki, Greece