Case by Dr. Salvatore Scolavino
After decades of developing and improving the matrix chemistry and filler technology contained in resinbased composites, the products available for direct restorative procedures finally seemed technically mature. What remained challenging, however, was the management of the extremely wide range of tooth shades and opacities available for each product: The dentin, body and enamel masses had to be selected and combined in the right way to obtain a perfect colour match and optical integration with the surrounding tooth structure. The difficulties associated with shade selection and calibration of layer thicknesses (particularly the top enamel layer) required to obtain the desired optical (desaturation) effects have now also finally been overcome.
The reason is that further improvements of the composites’ optical properties, mainly achieved through a careful selection and combination of fillers, have enabled the production of materials with optimized light diffusion properties. These properties enable the restorations to blend in smoothly with the adjacent tooth structure, thus paving the way for a single-shade concept (SSC). This concept involves the use of a single mass of composite to restore the function and aesthetics compromised by the loss of dental structure.
This translates into a significant saving of chair time and a high predictability of aesthetic outcome. A composite material supporting a single-shade technique needs to have medium opacity and a technology ensuring that the incoming light is absorbed, reflected and scattered in the right way to merge effortlessly with the surrounding natural dentition and create a biomimetic effect. The following clinical case reveals how the Light Diffusion Technology used in the CLEARFIL MAJESTY™ ES-2 Universal composite system (Kuraray Noritake Dental Inc.) leads to a highly predictable aesthetic integration obtained using the SSC.
Case description
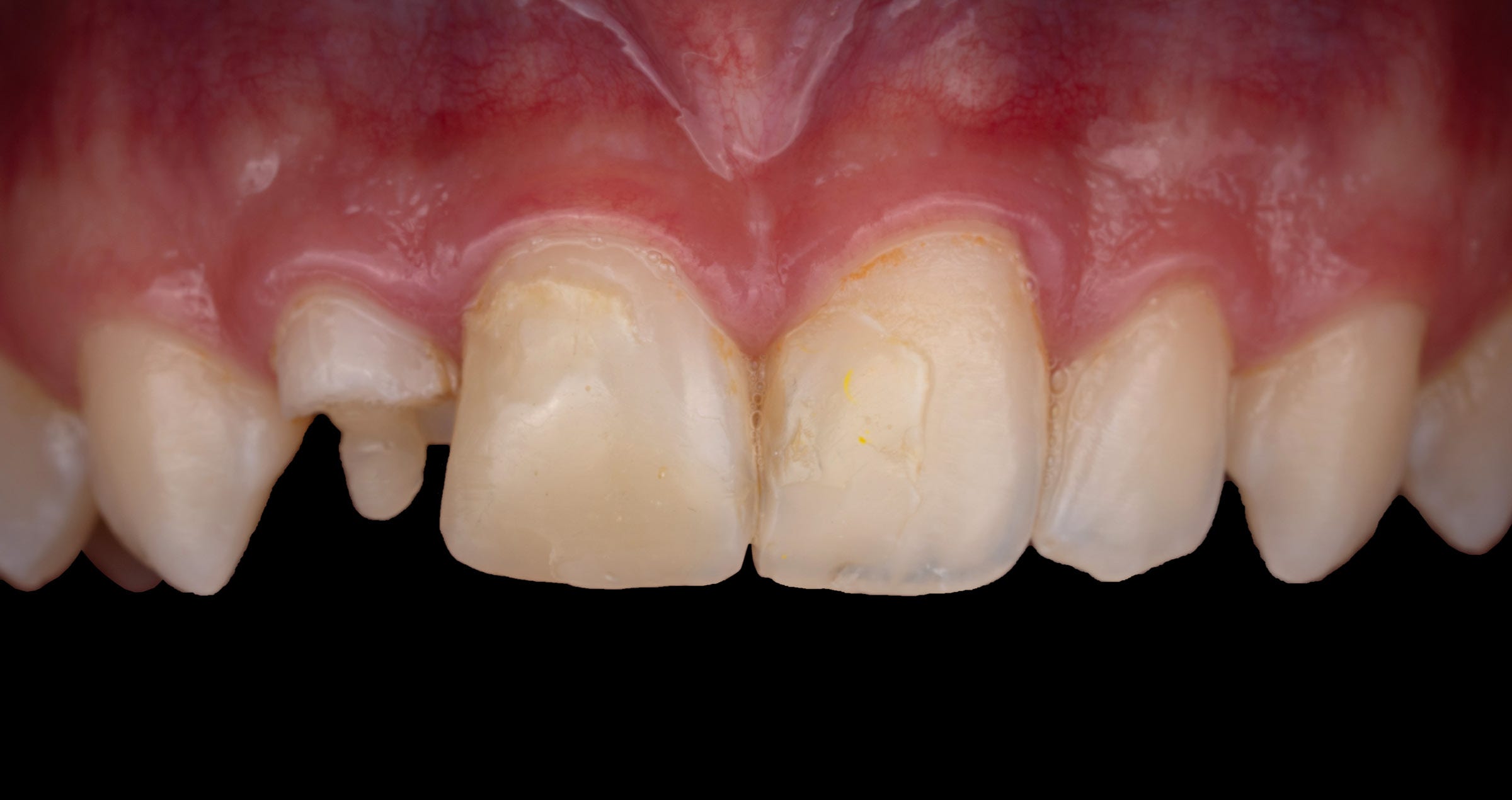
The 30-year-old female patient presented for a check-up, during which it appeared that her composite restorations in the second quadrant (the maxillary left first and second molar) needed to be replaced due to marginal leakage (Fig. 1). Once the rubber dam was in place (Fig. 2), the existing composite restorations were removed using a round multi-blade bur, which allowing for a selective removal of composite and carious tissue. The extension of the cavity was performed with a truncated cone diamond bur (fine). Once the cavity preparation was completed (Fig. 3), the enamel and dentin surfaces were cleaned by sandblasting with aluminium oxide (50 μm). Selective etching of the enamel was performed with K-ETCHANT Syringe (Kuraray Noritake Dental; Fig. 4), followed by thorough rinsing and drying of the tooth (Fig. 5). For the adhesive procedure with CLEARFIL™ SE BOND 2 (Kuraray Noritake Dental), the primer was applied first (Fig. 6), rubbed into the tooth surface for 40 seconds and air-dried. The bond was subsequently applied in the same manner (Fig. 7). After several seconds of air flowing to create homogeneous surface the adhesive was light-cured for 40 seconds (Fig. 8). As the last phase of the adhesive procedure, a 1-mm-thick layer of flowable composite (CLEARFIL MAJESTY™ ES-Flow Super Low A3, Kuraray Noritake Dental) was applied to cover the adhesive on the dentin (Figs. 9 and 10).
Fig. 1. Pre-operative clinical image.
Fig. 2. Isolation with rubber dam.
Fig. 3. First and second molar after cavity preparation.
Fig. 4. Selective etching of the enamel.
Fig. 5. Cavities ready for the adhesive procedure.
Fig. 6. Application of the tooth primer.
Fig. 7. Glossy appearance of the cavities after application of the bond.
Fig. 8. Light-curing of the adhesive layer.
Fig. 9. Application of flowable composite.
Fig. 10. Cusp-by-cusp modelling of the universal composite.
In the modelling phase, the posterior shade U of the composite CLEARFIL MAJESTY™ ES-2 Universal was placed using the cusp-by-cusp technique (Figs. 11 and 12). In order to improve the optical integration of the restorations, some brown stain (CHROMA ZONE™ COLOR STAIN Dark Brown, Kuraray Noritake Dental) was added to the fissures (Fig. 13). For finishing, we used a multi-blade ball-shaped bur and an Arkansas Flame abrasive stone (Fig. 14). Polishing of the restorations was accomplished with the TWIST™ DIA system (EVE; Fig. 15). After rubber dam removal, the occlusal check was performed with articulating paper (Fig. 16), minimal adjustments were made and the surfaces repolished. The integration of the restorations after 30 days fully meets the clinical expectations (Figs. 17 to 20).
Fig. 11. Glossy appearance of the cavities after application of the bond.
Fig. 12. Completed occlusal anatomy.
Fig. 13. Stained fissures.
Fig. 14. Matte surfaces after finishing.
Fig. 15. High-gloss surfaces after polishing.
FINAL SITUATION
Fig. 16. Whole quadrant after rubber dam removal and the occlusal check.
Fig. 17. Whole quadrant at the 1-month-recall.
Fig. 18. Occlusal view of the restorations …
Fig. 19. … after one month.
Conclusion
The innovative composite system CLEARFIL MAJESTY™ ES-2 Universal, which consists of two shades for the anterior and a single shade option for the posterior region, offers the properties needed for a successful implementation of the single shade technique. Used in the posterior region, the material is sufficiently opaque to mask optical irregularities of the underlying tooth structure, while it is translucent enough to provide for an imperceptible optical transition from the tooth structure to the restoration. Irrespective of the tooth shade, the restoration merges smoothly with the surrounding natural dentition, creating a harmonic overall picture.
Dentist:
DR. SALVATORE SCOLAVINO
Dr. Salvatore Scolavino, graduated with honors in Dentistry and Dental Prosthesis from the University of Naples. Dr. Salvatore is a specialist in aesthetics and direct and indirect anterior and posterior adhesive restorations. His focus lies with Conservation, Endodontics and Prosthetics in particular. He is an active member of prestigious academies and scientific societies: AIC -Italian Academy of Conservation, IAED -Italian Academy of Esthetic Dentistry and SIDOC (Italian Society of Conservative Dentistry. Since 2004, he has private practice Nola, Italy.
Dr. Scolavino is a founder of werestoreit.it, an inspiring site that offers abundance and variety of aesthetic clinical cases. Author of the book published by Quintessence Publishing „Direct Restorations in the posterior regions“, author of scientific publications in national and international journals, he is speaker at courses and conferences in Italy and abroad.